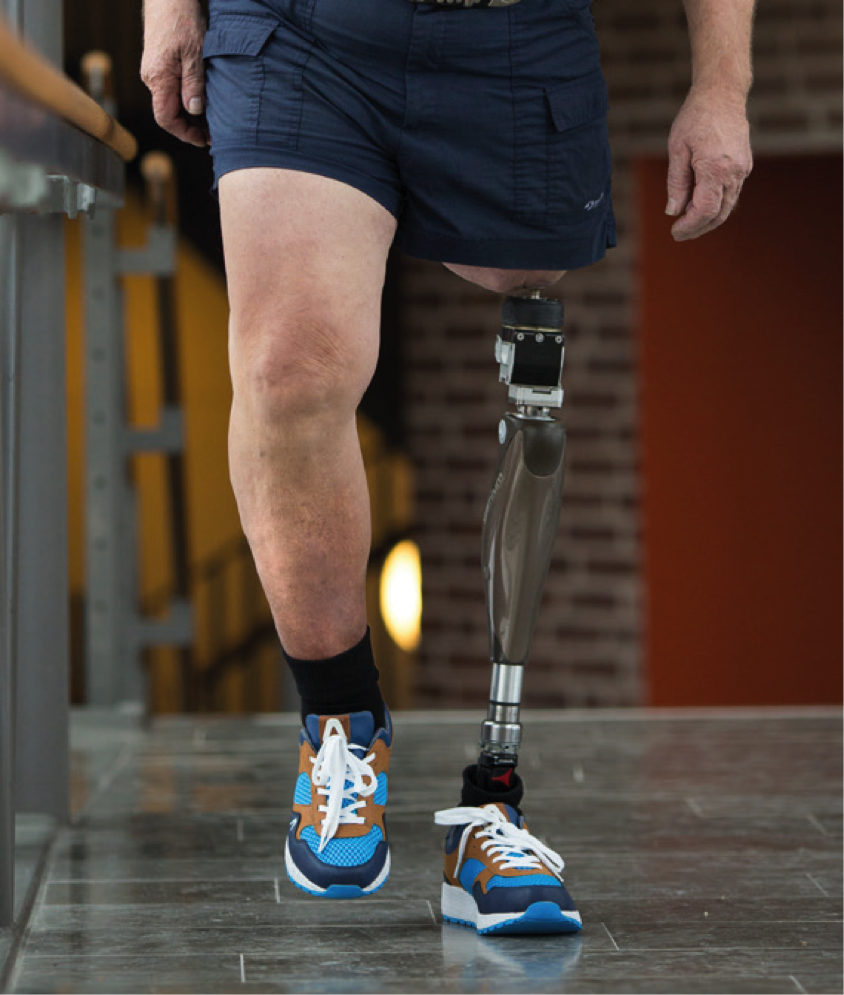
Grønt lys for osseointegrasjon i Norge

Osseointegrasjon ble oppfunnet i Göteborg på tidlig 80- tallet. I dag har Rikshospitalet fått grønt lys til å utføre behandlingen i Norge. De skal operere de aller første pasientene med god ekspertise fra Göteborg i Sverige allerede i desember og fra nyåret. Ortopedene ved Rikshospitalet ser fram til de aller første behandlingene av osseointegrasjon for […]
Ortopedene ved Rikshospitalet ser fram til de aller første behandlingene av osseointegrasjon for protesebrukere.
Av Marte Nordahl.
Magne Røkkum, Avdelingsleder og Professor ved Ortopedisk avdeling på Rikshospitalet, har ansvaret for all behandling av Villy Andresen. Magne har arbeidet som ortoped ved Kronprinsesse Märthas institutt og Rikshospitalet siden 1985.
– Det blir veldig spennende å få være med på det ortopediske inngrepet. Den nye behandlingsmetoden har vært i bruk i mange år i utlandet, spesielt i Gøteborg. Først nå har vi fått tillatelse fra staten å tilby osseointegrasjon i Norge. Her på Rikshospitalet vil vi følge opp disse pasientene systematisk for å se hvordan det går med dem, sier Magne Røkkum.
En kostbar metodikk
Magne informerer om at de har planlagt å operere de aller første pasientene først ved årsskiftet. Nå arbeider de med å samle opp egnede pasienter til denne operasjonen.
– Vi har allerede begynt å vurdere noen pasienter, og Villy Andresen er en av dem.
Vi vil få assistanse fra våre venner i Gøteborg med de første operasjonene, slik at vi er helt sikre på at de blir utført på en optimal måte, sier han.
– Hittil er det sannsynligvis mange pasienter i landet som kunne ha god nytte av en osseointegrert protese, men som ikke har fått tilbudet. Kun et begrenset antall pasienter har fått tillatelse til å utføre behandlingen i Gøteborg på den norske stats regning. At behandlingen er kostbar er litt av bakgrunnen for at vi nå har fått tillatelse med å utføre dette i Norge. Å gjennomføre behandlingen her i Norge, vil bli vesentlig billigere enn i Sverige. Dessuten blir det mindre belastende for pasienten.
Gammel svensk teknikk
-

Førsteamanuensis – Ortopedisk avdeling. Foto. Øystein Horgmo /UiO -
-
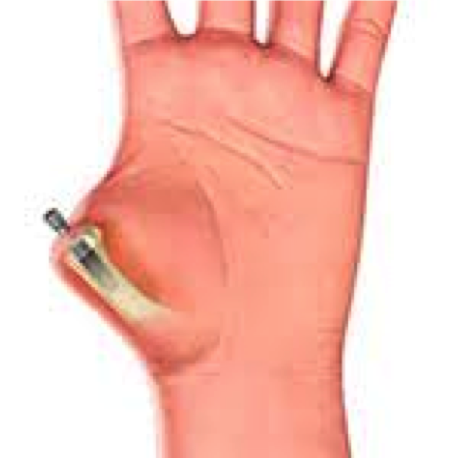
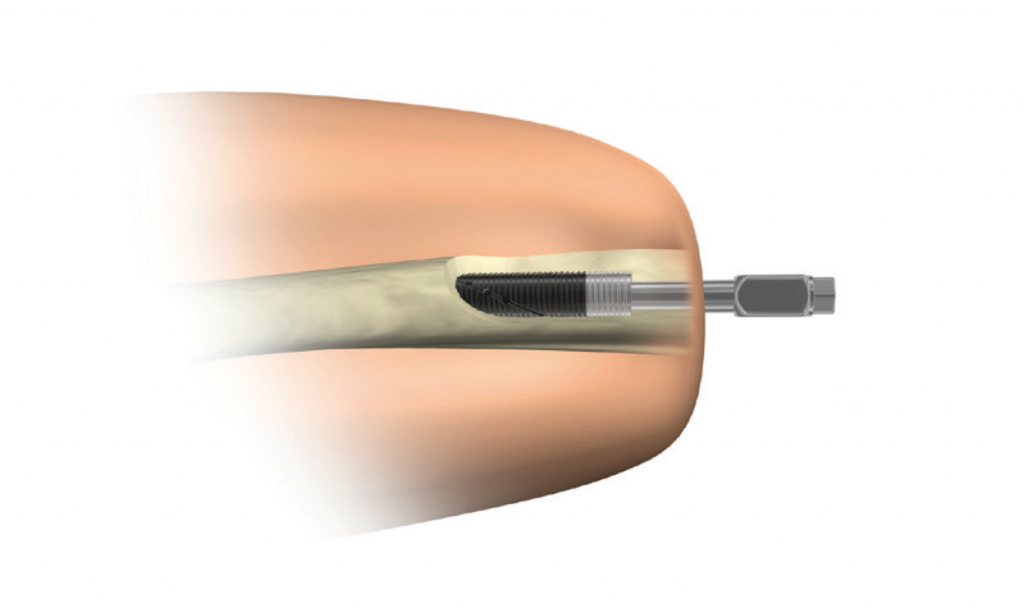
En bolt skrus inn i margkanalen på beinet i amputasjonsstumpen. Deretter lukkes hud og bløtdeler igjen. Etter en tid monteres det inn en ny bolt som går ut gjennom huden
Magne løfter fram det kompetanserike forskningsmiljøet i Gøteborg som hodene bak osseointegrasjon som metode, som ble oppdaget på 80- tallet.
– Jeg ble selv kjent med miljøet mens jeg tok doktorgraden for mange år siden. Forskerne fant ut at dersom de skrudde fast titan i skjelettet, vokste det fast uten at det dannet seg bindevevsmembran mellom metallet og beinet, informerer han.
Han løfter fram den kjente metoden som kalles for ”svensketenner”, som har blitt stor business. Titanskruer skrus inn i og skal sitte i 3-6 måneder, til det fester seg godt. Deretter festes tenner oppå skruene. Denne metoden brukes også til osseointegrasjon av proteser.
Opererer inn til skjelettet
– Vi starter med en operasjon hvor vi skrur inn en bolt i margkanalen på beinet i amputasjonsstumpen. Deretter lukkes hud og bløtdeler igjen. Etter en tid monteres det inn en ny bolt som går ut gjennom huden. Når området er leget og klart kobles det på en tradisjonell protese. Protesen blir da festet direkte i skjelettet gjennom bolten som er satt inn, utdyper han.
– Først etter 3-6 måneder vil bolten i beinet gro seg fast. Du vil gradvis kunne belaste beinet og ta i bruk den nye protesen over tid. Normalt sett vil det ta rundt ett år til du får tillatelse til å belaste beinet uten begrensninger. (I mellomtiden kan man bruke en vanlig protese), informerer Magne.
Korte amputasjonsstumper
Magne uthever at osseointegrasjon er mest velegnet for pasienter med korte amputasjonsstumper. Med en kort stump kan det være utfordrende å bære en vanlig hylse.
– Metoden er også egnet for pasienter som har problemer med å bruke tradisjonelle proteser av annen årsak. Eksempelvis de med arrvev og tendens til sårdannelse. Noen pasienter har også utfordringer med at amputasjonsstumpen varierer litt i størrelse, slik at protesen både kan oppleves for stor eller for trang. En del pasienter klager også over smerter og annet ubehag ved bruk av tradisjonelle hylseproteser. De kan også bli hjulpet av slike skjelettforankrede proteser, informerer Magne.
Lårbein og overarm
– En osseointegrert protese egner seg godt for de med amputerte lårbein og overarm. Løsningen kan også benyttes på legger og underarmer. Dernest finnes det også en variant som rekonstruerer tommelen, ved at man skrur inn en bolt i tommelresten. Når såret er leget blir det montert på en tommelprotese.
Magne utdyper at det som oftest er brukere som har vært i en ulykke eller utviklet svulst som velger en osseointegrert protese. Løsningen kan vurderes i andre tilfeller også. Endog er ikke protesene særlig aktuelle for bruker som har amputert beinet grunnet dårlig sirkulasjon eller sukkersyke (diabetes).
Enkel og fleksibel protesetype
Magne framhever at siden bolten er koblet direkte på skjelettet deres, opplever brukeren å få bedre styring og kontroll på protesen.
– Det er også mye enklere og raskere å smekke på denne protesen enn en tradisjonell hylse. Likedan er protesen plassert helt stabilt på skjelettet. Særlig yngre amputerte vil oppleve at denne løsningen gir mange mye aktivitetsmuligheter, sier han.
Utfordrende med infeksjon
– Selve operasjonen er ikke veldig vanskelig. Det er selvfølgelig et arbeid som krever nøyaktighet ut til fingerspissene. Men det er ikke blant de vanskeligste ortopediske operasjonene som vi utfører. Både det kirurgiske og tekniske knyttet til operasjonen er overkommelig.
– Ved innsetting av bolten anvender vi alle nødvendige tiltak for å slippe en infeksjon. Det er høyst sjeldent at det forekommer. Derimot kan det på lengre sikt krype inn bakterier mellom bolten og huden. Når det står en metallbolt ut gjennom huden, vil det alltid være en inngangsport til bakterier. Derfor kreves det en veldig streng hygiene. Allikevel er det en betydelig andel pasienter som får episoder med infeksjon. De aller fleste infeksjoner er overfladiske som kan løses med tradisjonell behandling med antibiotika. Det er sjeldent at det fører til at hele protesen svikter. Det verste som kan skje i så måte, er at infeksjonen løper inn til beinet hvor bolten er festet. Dette kan være vanskelig å bli kvitt. Heldigvis er de aller fleste infeksjonene overfladiske, og som man erfaringsmessig klarer å håndtere, informerer han.
15-20 pasienter i året
– I Sverige utfører de årlig rundt 30- 40 proteser med osseointegrasjon. Hvis de tallene er korrekte, kan det tenkes at vi vil utføre rundt 15-20 pasienter per år, informerer han.
– Det vil bli veldig spennende å se hvordan resultatet blir. Likeledes er det godt å arbeide med noe som vi tror kommer pasienten til nytte. Brukerne vi har vært i kontakt med som har fått en slik protese tilpasset i Sverige, har vært kjempefornøyd med operasjonen.
– Nå ser vi fram til å hjelpe Villy. Han er en positiv kar, og jeg har god grunn til å tro at dette vil gå bra. Får vi også inn flere aktuelle kandidater er vi positive til å ta dem imot, sier han.